Bruce Hastings, managing principal at De Mi Tierra Consulting and a former director of process technology at Amgen, highlights three fundamental mistakes often seen during packaging design for new treatments

Trial and error: even the most subtle differences in packaging for placebos could jeopardise trials
Pharmaceutical materials each have unique packaging requirements, and there are also several processes and systems to consider that can help to minimise delays and ensure swift deliveries. Bruce Hastings, managing principal at De Mi Tierra Consulting and former director of process technology at Amgen, discusses with Lyn Erb how packaging can optimise the efficiency of process.
The demands of pharmaceuticals are many and varied. Detailed planning and execution is critical to achieving optimal research outcomes, and compiling key product and patient data. Every aspect of pharmaceutical development needs to be meticulously orchestrated to ensure trial success – with packaging design and manufacture near the top of that list.
Packaging provides a unique challenge, one that is often neglected in terms of allocating the appropriate time, budget and logistical expertise required to safeguard the integrity of a pharmaceutical product.
The design and manufacture of packaging for clinical research does not present the same aesthetic or regulatory hurdles as in the commercial environment. However, getting it right can make or break a trial – and have a significant knock-on effect on the commercialisation of a therapy.
Study designs and trial protocols must consider practical, clear and user-friendly packaging that can be employed across multiple markets and study phases. Add in the cost implications of small-scale production, and the challenges of blind-testing, and randomisation across different sites and international borders, and the importance of a detailed packaging strategy becomes clear.
Bruce Hastings, managing principal at De Mi Tierra Consulting and a former director of process technology at Amgen, highlights three fundamental mistakes often seen during packaging design for new treatments.
“A lack of planning, combined with tight time restraints, can often lead research teams to accept a less-than-optimal design,” he says. “Secondly, a basic lack of understanding of the users, their needs and a failure to design for them can affect outcomes.
“Thirdly, there is often a lack of optimal packaging, in terms of volume, that is qualified and production-ready.”
Pharmaceutical packaging to protect delivery integrity
Helping to preserve the integrity of a clinical trial, an integral aspect of drug development, should be a fundamental objective of packaging. Poor packaging can inadvertently ‘unblind’ trials and put at risk years of research and investment. A slight variation in the colour of a placebo packet compared with the product packet, different adhesives or shortcuts on labelling can all affect trial outcomes.
Hastings says trial participants often go to extraordinary efforts to identify whether they are being given a placebo or the trial drug.
“You would be amazed how they try to defeat efforts to keep them in the dark,” he says.
Substandard labelling or using a label and adhesive combination that is not aggressive enough is a common error.
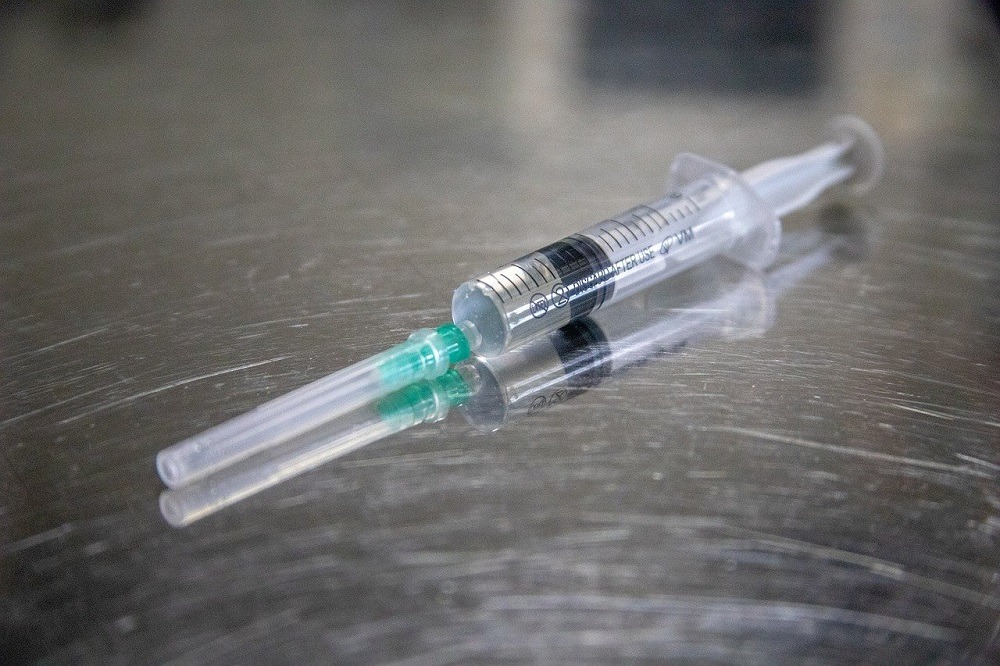
To protect trial integrity, however, medication must not only be blind to patients, but also to medical practitioners dispensing the drug and placebos, and to researchers analysing the results. Medications and placebos, along with all components and materials used in packaging – including blister packs, bottles, closures, caps, vials and ampoules – must be identical. Supplementary materials used during mode of administration, such as syringes or injection pens, must also be foolproof.
“The packaging demands typically depend on the trial phase you are in,” explains Hastings. “In phase one – and sometimes into phase two – packaging tends to be very basic, and typically based on the manufacturer’s existing capabilities and pack options.”
Hastings says that while there is no obligation to progress or develop packaging as a trial advances, phase three can provide sponsors with an opportunity to road test commercial primary packaging in real-world environments.
“This is a marvellous opportunity to gain some insight from users, and it can be invaluable in the design of the secondary packaging in terms of facilitating intuitive or correct use,” he says. “The big difference in phase three is that it is about user interface – do we need a design to assist in titration? What are the needs in terms of blind-testing, serialisation or comparative studies? These can all change the secondary look.”
He says these requirements in a clinical space can be very different to the demand of a future commercial space.
Serial offending
Serialisation is another core consideration during each of the trial phases, and is key to tracking medication use and recording test results. Without a protocol to safeguard data, it is impossible to safeguard trial integrity.
Hastings says missing serialisation numbers or the misinterpretation of numbers can often be linked back to poor packaging design and printing.
Attention to consistency and accuracy – especially across batches or in preparation for expanded trials – during the design and manufacturing process can help eliminate these concerns.
Packaging can also differ depending on the trial requirements and goals. Labelling – and its influence on functionality – is of particular concern when combination products are being tested. “There is always a need for human factors testing for a combination product,” Hastings says. “By this I mean the need to prove the design facilitates the correct use of the product.”
Trials of combination products are focused much more on the needs of the user and the need to gather data on successful use of the product, in addition to the actual product efficacy.
“This has driven us to think much differently on the secondary packaging design for combination product trials, with less hiding of the product and more emphasis on facilitating use,” says Hastings.
In this respect, approvals and regulatory processes for packaging are usually of secondary importance to trial integrity, efficacy and collating user data when it comes to measuring trial outcomes.
“Labelling in trials, for example, is much more study facilitator-focused, as opposed to in the commercial environment, where you have to satisfy the regulatory agencies, physicians, pharmacists and users,” explains Hastings.
Supply chain strategies
Even so, poor design can affect the integrity of all trials – not just blind trials – and there are areas in which packaging for medical trials requires the same robust protections that are present in the commercial arena. Protecting all medication and materials against damage during shipping and storage is one obvious example.
Whereas large-molecule medications are more reliant on cold shipment and storage, small-molecule therapies are more robust. Expiration dates and shelf life are other important considerations, especially across multiphase or extended trials, or when trialling expensive biologics that may have a limited used-by date. Packaging designers need to cover all supply chain eventualities that may arise over the life of the trial – from mitigating the impact of lower volumes and higher costs for smaller trials, to having strategies that manage unexpected or suboptimal trial enrolments, and the consistency of packaging across delayed or extended phases of research. Not only do these challenges have budgetary implications, they can also affect trial integrity.
“You need to have a strategy for your pipeline so you can solve these types of issues,” says Hastings. “If you don’t, you end up scrambling for solutions that are less than optimal.”
He says it can be a good idea to create standard packaging target designs of different sizes for specific product lines.
“For example, HDPE [high-density polyethylene] bottles for small-molecule [and] vials for steriles and biologics,” Hastings explains. “These would be designed for production lines and be pre-qualified on them.”

The nick of time
Trial designers are increasingly experimenting with just-in-time (JIT) manufacturing and customisation to minimise some of the costs related to smaller or multicentre trials. “There is potential for reducing costs and adding flexibility with the JIT concepts, as you can more efficiently direct supply to studies where enrolment is higher than expected versus having a pre-labelled product that is not used due to low study enrolment,” says Hastings.
Such innovations should be written into trial protocols to safeguard processes for utilising partially packaged products that are labelled and shipped on demand. Here, the identification and tracking of products can pose additional challenges if tight guidelines are not followed.
Regardless of the protocol adopted, reliable and efficient manufacturing partners are essential.
Hasting advises utilising standard equipment technologies that can be easily adapted from low to high-speed manufacturing. These often start out as small work cells with manual transfers between activities, but they should be based on technology that can been automated as and when required.
“The small high-mix, low-volume-type packaging areas can be very flexible and adaptable to the need of most trials, yet the technology is scalable to higher speed and capacity,” he says.
“A lack of these solutions can lead to running inefficiently on high-speed lines and wearing the high costs that can be involved.”
This article originally appeared in the Spring/Summer 2020 edition of Packaging Today. The full issue can be viewed here.
